Heart Disease Risk: The Latest On Cholesterol Learn the flawed methodology used to increasingly prescribe statin drugs and why the true culprit (or culprits) often remains undiagnosed.
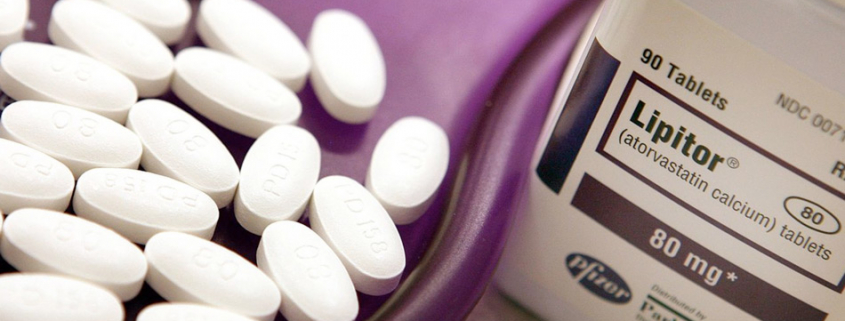
Cholesterol has been vilified for years as the top contributor to cardiovascular disease (CVD) and chronic heart disease (CHD), to the point where lowering that number has practically become a national obsession. The medical community’s answer to this is to prescribe statin medications, like Lipitor, which have dangerous, sometimes permanent side effects.
This obsession comes at a high cost: First, the number of people being prescribed statins for the wrong reason increases every year as pharmaceutical companies press laboratories (and doctors) to further tighten the acceptable range for cholesterol. Even children as young as eight years old are being indoctrinated to The Cholesterol Myth and are being prescribed statins instead of really taking into consideration what would have better long term health benefit for these young lives.
And sweeping recommendations that everyone over fifty should automatically be put on statins “as life-savers” to prevent cardiovascular disease is frightening and not supported in the research. What most patients don’t realize is that cholesterol itself is cardioprotective. When the arterial walls are plaquing it is not because cholesterol manufacture has run amok; in fact, arterial plaquing is a result of thinning and fragility, a weakness in the arterial walls themselves that need shoring. Think of cholesterol as a patch; the same kind of patch used to repair a leaky, punctured tire.
Not only that, cholesterol aids in hormone production as it sits atop the cascade of hormones beneath it, at the very apex of all hormones that are essential to reproduction and survival. It is also a structural component of cells (it is the lipid membrane that constitutes the cell wall), and plays a role in digestion. In fact, cholesterol is so essential that approximately 80 percent of it is manufactured in the liver while only a minor percentage comes from the foods we eat. Think about why that is? When our diet doesn’t contain enough cholesterol, our body will try to make up for the shortage by manufacturing more of it in the liver. Indeed, a very low cholesterol count is associated with a number of serious health problems including cancer, depression, anxiety and more.
A Better Way
Fortunately, today there is great division within the medical community, with a number of highly respected medical professionals questioning the risk-benefit ratio of statins and pointing out the “flawed methodology”, “industry sponsorship” and “statistical deception” used to evaluate the effectiveness and safety of statins. It’s about time!
In approaching the body’s hormone and heart chemistry from a functional medicine perspective, cholesterol is not only necessary, it is essential. It is the precursor to all other hormones, including the steroid hormones such as cortisol and the reproductive hormones like estrogen, progesterone and testosterone.
By obsessing over cholesterol, patients are missing three important facts:
- True risk of heart disease requires a number of markers to properly evaluate (before taking statins), including epigenetic and inflammatory markers, not just cholesterol, and is generally a function of other co-morbidity factors like high blood pressure and a history of diabetes.
- 50 to 75% of patients hospitalized with an acute myocardial infarction (heart attack) have normal cholesterol levels as defined by traditional medical standards (lipid measurements).
- A significant number of heart disease cases are autoimmune and a result of systemic inflammation unrelated to cholesterol.
So what’s the real culprit?
New studies reported by the Royal Pharmaceutical Society Journal show strong evidence that it is insulin resistance, and not cholesterol, that is at the root of cardiovascular disease. This is true for Type 2 diabetes and obesity, as well. In fact, populations in the US and around the world were studied and it was found that body mass index, weight and cholesterol were “ineffective”, “inconsistent” or “misguided” as risk markers for heart disease, obesity and Type 2 diabetes.
Trouble is, there is no medication to reverse insulin resistance. Medications prescribed to improve insulin sensitivity have been only mildly successful, and one type of drug is reported to have actually increased mortality in patients with Type 2 diabetes.
Likewise, it was also discovered that instead of focusing solely on caloric intake, which is commonly the case for anyone overweight or diabetic, or suffering with chronic hypertension, the important factor was whether the calories were coming from processed foods or whole foods. In other words, nutrient dense calories and junk calories are not equal; it’s the metabolic changes that result from eating healthy food that matters.
One such study, the Lyon Diet Heart Study, looked at the effects of different types of food on insulin resistance and found that the Mediterranean diet, which is filled with healthy fats and fresh vegetables, was one of the best for heart health. The conclusion was heart disease risks need to be redefined, and that “lifestyle interventions” were by far more successful than drug interventions.
Be Smarter
Viruses are here to stay; they’ve always been around us, but Covid-19 has made us more aware of their potential severity and the corrosive effect it has on patients with underlying blood vessel diseases. Aside from wearing a mask and social distancing, one of the best strategies to focus on right now for all of us is strengthening our immune systems and our health.
For patients with underlying autoimmune disease, heart disease, chronic illness, or who want to focus on performance, we also recommend testing for specific areas of weakness, including genetic weaknesses, to help identify and restore improvements for future-proofing against viruses that arrive on our doorsteps.
Dr. Doug Pucci is a functional medicine practitioner who was honored in 2020 to receive both The Best Of 2020 Awards for Functional Medicine in Oradell, NJ, and entry into Trademark Publications’ Who’s Who Directory, Honors Edition, for his pioneering work. He provides comprehensive testing for health biomarkers, advanced discovery into brain/body well-being and personalized nutrition for a diversity of people and symptoms.
For more information, call 201-261-5430 or visit GetWell-Now.com